If you’re in the medical billing and coding field, particularly for wound care, understanding and accurately using the right CPT (Current Procedural Terminology) codes is essential.
Wound care coding can be tricky, but with the right knowledge, you can avoid common pitfalls and ensure better reimbursement.
This guide will walk you through the essential CPT codes for wound care, including debridement, dressing changes, telehealth services, and more.
Wound care coding focuses on billing for medical services related to the treatment of injuries, ulcers, and surgical wounds.
Wound care requires rigorous adherence to payer guidelines.
It includes documentation of wound status, treatment, and progress, and accurate and detailed coding.
Accurate coding in wound care ensures proper reimbursement for services and procedures such as debridement, wound repair, and evaluation and management (E/M) services.
Different types of wounds require different codes, and there are specific guidelines to follow.
Importance of Precise CPT Usage
Correctly selecting CPT codes in wound care is crucial for accurate billing and proper reimbursement.
Misuse of codes can lead to claim denials, delayed payments, or even audits.
For example, using the wrong code for wound debridement or dressing changes can result in lower reimbursement rates or a complete denial from insurers, including Medicare.
Knowing common wound care CPT codes is essential for wound care practices and providers.
This ensures you don’t miss out on reimbursement opportunities.
Some most commonly used CPT codes in wound care are:
- 97597: This code is used for selective debridement of wounds, which involves removing necrotic tissue to promote healing.
- 97598: Similar to 97597, this code is for the second unit of selective debridement when done in more extensive sessions.
- 11042, 11043, 11044: These codes are for surgical wound debridement, with the number indicating the depth of tissue removed. They cover superficial to deep tissue debridement.
Wound debridement is one of the most frequent procedures in wound care. The right code depends on the type and depth of the debridement performed.
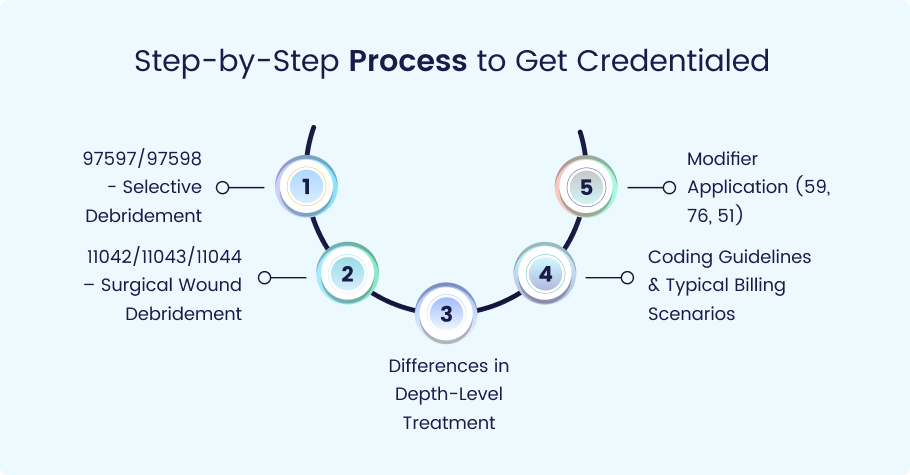
97597/97598 – Selective Debridement
Selective debridement refers to the removal of dead or infected tissue while preserving healthy tissue. Usually, this happens in outpatient settings or during wound care visits. Healthcare providers use this code to bill small to medium-sized wounds..
Example:
If a patient has a diabetic ulcer and the doctor removes only necrotic tissue without disturbing the healthy skin, they will use CPT 97597 for the first unit and 97598 for any additional unit.
11042/11043/11044 – Surgical Wound Debridement
These codes are for more invasive procedures, where a surgeon removes tissue from deep wounds or ulcers.
- 11042: For superficial wounds (just under the skin).
- 11043: For intermediate wounds (involving muscle or fascia).
- 11044: For deep wounds (involving muscle, bone, or other deep tissue).
Usually, hospital or surgical center settings use these codes in claim filing.
Differences in Depth-Level Treatment
- 11042: May apply to a wound like a minor surgical incision.
- 11043: Used when the wound is deeper, like a wound involving muscle.
- 11044: Reserved for severe wounds involving muscle, fascia, or bone.
Coding Guidelines & Typical Billing Scenarios
- Always use the appropriate code based on the depth of tissue removed.
- Include proper documentation of the wound’s size and depth, as it supports accurate billing.
Modifier Application (59, 76, 51)
Modifiers help to clarify specific conditions of a procedure:
- Modifier 59: Indicates that a procedure was distinct or separate from other procedures.
- Modifier 76: Used when a procedure is repeated by the same provider.
- Modifier 51: For multiple procedures performed during the same session.
Example:
If you perform both 97597 (selective debridement) and 11042 (surgical debridement) during the same visit, you might use modifier 59 to indicate that the two procedures were distinct.
Changing a wound dressing is a critical component of wound care. There are specific CPT and HCPCS codes for different types of dressing changes.
97602 – Non-Selective Debridement
Medical providers utilize this code for non-selective debridement, where the goal is to clean the wound but not selectively remove necrotic tissue. It often applies to larger or more complex wounds.
97535 – Custom Ongoing Dressing Change
This code covers the ongoing changes of dressings in chronic or large wounds. It typically includes customizing dressings to the patient’s needs.
A4011/A4012 HCPCS Supply Codes
These HCPCS codes cover wound care supplies, like bandages and dressings. Properly coding the supplies ensures that these costs are reimbursed.
When coding for wound care, it’s important to understand the difference between timed and untimed services.
Semantics of Unit Reporting
- Timed Services: These are billed based on the time spent performing a procedure. For example, if debridement takes 30 minutes, the provider might bill for one unit of a timed service.
- Untimed Services: These are billed as a single unit regardless of time. For example, CPT 97597 for debridement might be billed as one unit even if the procedure takes 15 minutes or 60 minutes.
Combination Claims: Blending E/M + Debridement
Many wound care visits involve both Evaluation & Management (E/M) codes (for the assessment) and debridement. When billing, ensure you correctly combine the codes to reflect both the assessment and the procedure.
Telehealth for wound care is growing in popularity, especially with remote monitoring.
Using Modifiers 95, GT
- Modifier 95: Used for telehealth services, indicating that the service was delivered remotely.
- Modifier GT: Indicates the use of video communication for remote care.
Remote Monitoring CPT Guidance
For remote wound care, the coding usually involves time-based services for monitoring or consultations. Always check with your payer to ensure compliance with specific telehealth guidelines.
Medical Necessity Thresholds
For reimbursement, providers must demonstrate the medical necessity of the wound care treatment. Document patient’s history, wound type, and treatment plan accurately.
Including Wound Size, Stage, Location
The wound’s size, stage, and location play a key role in coding. For example, a diabetic foot ulcer (ICD-10 code E11.621) might require more intensive care than a superficial cut.
Avoiding Bundling Errors per LCD/NCCI
The National Correct Coding Initiative (NCCI) prevents inappropriate bundling of codes. Make sure to review NCCI edits before submitting claims to avoid bundling errors.
NCCI edits ensure that billing is accurate. Remember, you can’t bill certain code pairs together like 11042 and 11200 before they meet specific criteria.
Key Edit Pairs (e.g., 11042 with 11200)
According to NCCI Edits rules, these code pairs (unable to bill together) are CPT 11042 (surgical debridement) and 11200 (removal of foreign body).
So, you cannot bill them together unless you don’t document them accurately.
How to Check and Override Edits
You can check NCCI edits via the CMS website or your coding software. In cases where a code pair is denied, you might need to file an appeal with supporting documentation.
Understanding Medicare’s reimbursement rates and LCD policies is essential for accurate billing.
Typical 2025 Reimbursement Benchmarks
Reimbursement rates can vary based on the type of service and location. For example, debridement might have a higher reimbursement rate than basic dressing changes. It’s important to stay updated on these rates.
Checking LCD Policies by Medicare Administrative Contractor (MAC)
Medicare’s LCDs provide information that covers these codes in specific regions. Ensure you’re familiar with the LCDs from your region’s MAC to avoid claim denials.
Why Outsource Wound Care Billing to Medheave?
Outsourcing your wound care billing can save time and reduce errors. Medheave provides:
- AAPC/AHIMA-certified medical coders who understand the intricacies of wound care.
- Increased first-pass claim acceptance, reducing time spent on re-submissions.
- Faster payment cycles and effective denial recovery.
- Full Revenue Cycle Management (RCM) integration, covering eligibility, billing, and accounts receivable.
Conclusion
Accurate wound care CPT codes are essential for ensuring proper reimbursement for services rendered.
Whether you are handling wound debridement CPT codes, wound dressing changes, or navigating Medicare billing rules, the key is to follow coding guidelines and stay up-to-date on local coverage policies.
Implementing best practices for documentation and modifier usage can help you avoid common billing mistakes and reduce claim denials.
By outsourcing your wound care billing to experienced professionals like Medheave, you can save time, increase claim acceptance rates, and focus more on patient care.
This ensures that you not only get reimbursed properly but also run a smoother operation with less hassle.
Frequently Asked Questions (FAQs)
What is the difference between 97597 and 11042?
- 97597 is for selective debridement, whereas 11042 is for surgical wound debridement. The key difference is that 97597 is less invasive and typically used for smaller wounds.
How can I avoid wound care claim denials?
To avoid wound care claim denials, ensure that your documentation is thorough and includes the necessary details such as wound size, depth, location, and stage.
Always check the latest National Correct Coding Initiative (NCCI) edits to ensure you’re not bundling codes incorrectly.
Also, be sure to follow Medicare Local Coverage Determinations (LCDs) to confirm that the codes you’re using have insurance coverage in your area..
What modifiers should I use for wound care services?
- Modifier 59 is used to indicate that a service is distinct or separate from other procedures.
- Modifier 76 is used when a procedure is repeated by the same provider.
- Modifier 51 is used for multiple procedures performed during the same session.
- For telehealth services, you’ll use modifier 95 or GT depending on the platform.
Are there specific codes for wound dressing changes?
Yes, there are specific CPT codes for dressing changes. For instance, CPT 97535 is often used for custom ongoing dressing changes. Additionally, HCPCS codes A4011 and A4012 are used to cover wound care supplies like bandages and dressings.
How do timed vs untimed services affect wound care billing?
Timed services are usually billable based on the duration of the procedure. For example, debridement might be billed by the time spent, such as a 30-minute session.
On the other hand, untimed services, like certain debridement codes, which you can bill per unit, regardless of how long the procedure takes.
Can I bill for wound care services under telehealth?
Yes, you can bill telehealth services for wound care that meet specific requirements. You’ll need to use modifiers like modifier 95 or GT to indicate remote services, and you may also need to follow specific guidelines for remote monitoring.
What is the importance of using the correct ICD-10 codes for wound care?
Correct ICD-10 codes (such as L97 for diabetic ulcers or I10 for hypertension) are crucial because they support the medical necessity of the wound care provided. Accurate ICD-10 coding ensures that your claim is in line with the diagnosis and justifies the need for treatment.